Our Revolutionary Lineup Of Courses
View our courses
- Dry Needling
- Manual Therapy & Clinical Reasoning
- Digital Education
Category: Dry Needling
Integrated Clinical Dry Needling Total Body Level 1
Register here
The Integrated Clinical Dry Total Body Needling Course 1 provides clinicians with a comprehensive foundation in dry needling, including its historical context, proposed mechanisms, and current evidence supporting clinical use. Participants will develop proficiency in needle handling, CDC safety standards, pain education principles, and the clinical application of dry needling techniques for the most commonly treated and clinically relevant muscles.
The course also addresses state-specific rules and regulations governing dry needling practice. Clinicians will learn how to integrate foundational pain science concepts into real-world clinical decision-making. Instruction includes a detailed review of trigger points, patient positioning, and relevant anatomy — including vasculature, nervous tissue, and viscera — alongside safe and effective dry needling techniques and needle handling for all listed muscles.
This course is designed to support clinicians in delivering precise, informed, and responsible dry needling care grounded in anatomy, safety, and clinical reasoning.
The Integrated Clinical Dry Needling Course 2 is the second course in the two-part certification series and builds upon the foundational principles established in Course 1. This course provides clinicians with a deeper understanding of the history of dry needling, proposed mechanisms, and current evidence supporting its clinical utilization. Emphasis is placed on advanced needle handling and safety considerations, pain education, and the clinical application of dry needling techniques.
State-specific rules and regulations governing dry needling practice are reviewed to ensure safe, compliant application in clinical settings. Participants will further integrate foundational pain science concepts into real-world clinical decision-making.
Instruction includes an expanded review of trigger points, patient positioning, and relevant anatomy — including vasculature, nervous tissue, and viscera — along with dry needling techniques and needle handling for all previously introduced muscles as well as more advanced musculature.
Completion of Course 2 fulfills the requirements to complete the Dry Needling Certification.
Category: Manual Therapy
From Surgery to Sport: ACL Injury Rehabilitation With the Finish Line in Focus

A Revolution in Rehabilitation
Most ACL rehab courses teach you what to do.
This one teaches you how to think.
Join Dr. Luke Bunch, board-certified Orthopedic and Sports Physical Therapist and ACL rehab specialist, as he breaks open the black box of ACL recovery, from initial injury and early post-op decision-making to real-world return-to-sport demands.
With years of experience treating ligamentous knee injuries and mentoring rehab professionals, Dr. Bunch shares hard-earned insights that don’t live in protocols or timelines. You’ll gain practical skills, sharper clinical judgment, and a deeper understanding of how to guide athletes through one of the most challenging injuries in sports medicine.
Beyond clinical practice, Dr. Bunch is actively involved in ACL research and collaborates with leading clinicians and researchers across the country and internationally. His approach is grounded not only in day-to-day patient care, but also in ongoing scientific inquiry and dialogue with those shaping the future of ACL rehabilitation.
Learn how to think differently about ACL rehabilitation and change your outcomes.
Category: Manual Therapy
Unified Care: Integrated Clinical Reasoning and Patient Management for the PT/PTA Team
Physical Therapists and Physical Therapist Assistants work together across the full continuum of patient care. As research evolves and expectations rise, translating current best evidence into consistent, effective clinical practice can be challenging — especially within team-based environments.
The Unified Care: Integrated Clinical Reasoning and Patient Management for the PT/PTA Team course is designed to align physical therapists and physical therapist assistants around a shared framework for patient care. Emphasis is placed on continuity of care, effective pain education, strong therapeutic alliance, and the use of clear, appropriate language and communication to support optimal outcomes.
This 70% lab-based, two-day course integrates current evidence with clinical reasoning and hands-on manual therapy techniques for both peripheral and spinal joints. Participants will develop shared expectations, refine communication strategies, and practice manual skills that support cohesive, patient-centered care.
By the end of the course, participants will be able to immediately integrate evidence-informed clinical reasoning, manual therapy, and pain science education — working together as a unified team to deliver consistent, high-quality patient care.
Great outcomes don’t come from isolated providers — they come from unified care.
The Total Joint Post-Operative Care: Current Concepts and Best Practices course is a two-day experience designed to support evidence-informed assessment and treatment of post-surgical joint replacement patients. Through a combination of focused didactic instruction and hands-on technique labs, participants will expand their clinical skill set and exercise prescription strategies to influence muscle recruitment, tissue healing, and pain modulation — with the goal of improving functional mobility.
Participants will be guided through multiple examples of post-operative protocols, including stage-specific goals and progression strategies across the healing continuum. Emphasis is placed on understanding why and when to apply specific interventions, rather than simply following timelines.
By the end of the course, clinicians will be able to immediately integrate current best evidence, clinical reasoning, manual therapy, and pain science education into their existing rehabilitation approach for patients following joint replacement surgery.
Post-operative care isn’t about doing more — it’s about doing what matters, at the right time.
Category: Manual Therapy
Integrated Clinical Reasoning and Treatment of Dysfunctions: Lumbar Spine, Hip and Lower Extremity
Conditions involving the lumbar spine and lower extremity are a common source of pain, movement dysfunction, and long-term functional limitation. Effective care requires integrated clinical reasoning, skilled manual therapy, and movement strategies that address the system as a whole.
The Integrated Clinical Reasoning and Treatment of Dysfunctions: Lumbar Spine, Hip, and Lower Extremity course is a 70% lab-based, two-day experience designed to integrate current best evidence with decision-making frameworks and hands-on treatment. Participants will develop proficiency in manual therapy techniques — including joint mobilizations, high-velocity low-amplitude thrust techniques, neural mobilizations — alongside targeted exercise-based interventions for lumbar and lower extremity dysfunctions.
This course emphasizes immediate clinical application. Participants will learn how to assess, treat, and progress patients with lumbar spine, hip, knee, and ankle conditions using evidence-informed clinical reasoning. Foundational pain science concepts are integrated throughout to support thoughtful, patient-centered care.
By the end of the course, clinicians will be equipped to confidently apply current best evidence, manual therapy, and exercise strategies to improve function across the lumbar spine and lower extremity.
Lower quarter care isn’t about isolated joints — it’s about how the system moves, adapts, and recovers.
Conditions involving the cervical and lumbar spine are a leading source of pain, functional limitation, and long-term disability. Effective care requires more than isolated techniques — it demands integrated clinical reasoning, skilled hands-on treatment, and movement-based solutions.
The Integrated Clinical Reasoning and Treatment of Dysfunctions: Total Spine course is a 70% lab-based, two-day experience designed to bridge evidence, decision-making, and hands-on care for patients with cervical and lumbar spine dysfunction. Participants will integrate current best evidence with manual therapy interventions — including joint mobilizations, high-velocity low-amplitude thrust techniques, neural mobilizations — and targeted exercise-based strategies.
This course is built to support immediate clinical application. Participants will develop a clearer framework for assessment and treatment, refine manual skills, and learn how to integrate foundational pain science concepts into everyday clinical practice.
By the end of the course, clinicians will be equipped to confidently evaluate, treat, and progress patients with cervical and lumbar spine conditions using a thoughtful, evidence-informed, and human-centered approach.
Category: Manual Therapy
Integrated Clinical Reasoning and Treatment of Dysfunctions: Lumber Spine and Hip Region

Conditions involving the lumbar spine and the lower extremity frequently lead to impairments contributing to significant disabilities and functional limitations. This course is a 70% lab-based course integrating the latest evidence and frame work for decision making, and manual therapy for joints including high-velocity low-amplitude thrust techniques, neural mobilizations, and exercise based interventions for patients with lumbar and hip dysfunctions.
This 2-day course will enable the participant to understand and immediately integrate current best evidence, clinical reasoning, manual therapy, and exercises for the lumbar spine and hip. Additionally, they will be able to integrate the basics of pain sciences into their clinical practices.
Category: Manual Therapy
Integrated Clinical Reasoning and Treatment of Dysfunctions: Cervical and Thoracic Spine, Shoulder and Upper Extremity

Conditions involving the cervical and thoracic spine, shoulder, and upper extremity are a common source of pain, movement dysfunction, and functional limitation. Effective care requires integrated clinical reasoning, skilled manual therapy, and movement strategies that address the upper quarter as a connected system.
The Integrated Clinical Reasoning and Treatment of Dysfunctions: Cervical and Thoracic Spine, Shoulder, and Upper Extremity course is a two-day, lab-based experience designed to integrate current best evidence with decision-making frameworks and hands-on treatment. Participants will develop proficiency in manual therapy techniques — including joint mobilizations, high-velocity low-amplitude thrust techniques, neural mobilizations — alongside targeted exercise-based interventions for cervico-thoracic, shoulder, and upper extremity dysfunctions.
This course emphasizes immediate clinical application. Participants will learn how to assess, treat, and progress patients with cervical spine, shoulder, elbow, wrist, and hand conditions using evidence-informed clinical reasoning. Foundational pain science concepts are integrated throughout to support thoughtful, patient-centered care.
By the end of the course, clinicians will be equipped to confidently apply current best evidence, manual therapy, and exercise strategies to improve function across the cervical spine and upper extremity.
Upper quarter care isn’t about isolated regions — it’s about how the system communicates, stabilizes, and moves.
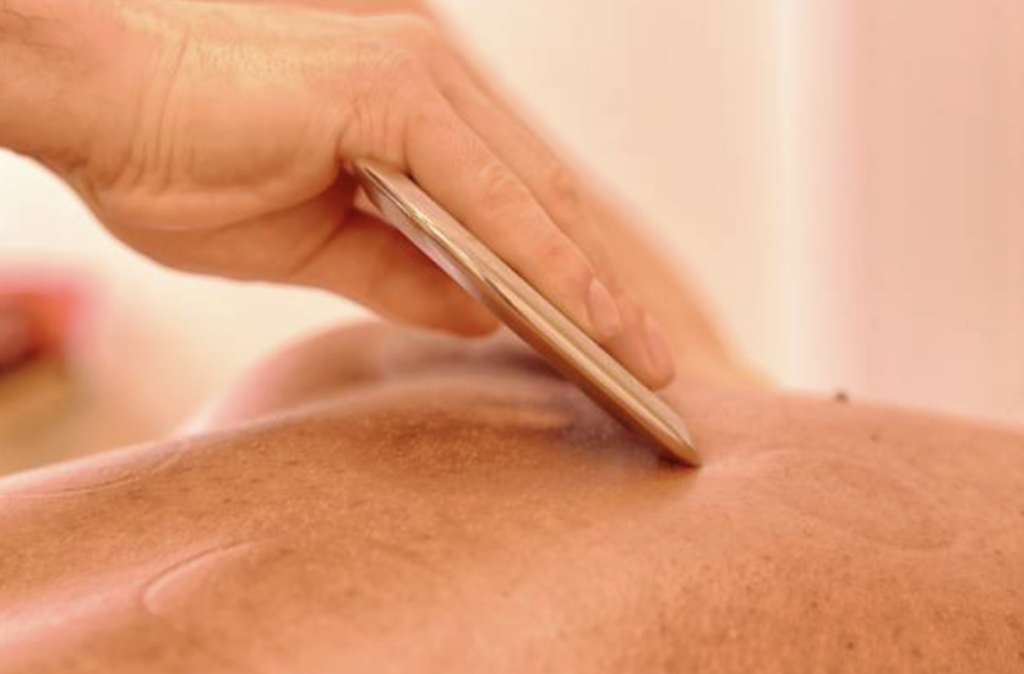
Instrument Assisted Soft Tissue Mobilization (IASTM) is a commonly used intervention across many clinical professions. As research evolves, effectively integrating current best evidence into day-to-day practice requires thoughtful clinical reasoning, clear communication, and consistent patient-centered care.
The Instrument Assisted Soft Tissue Mobilization course is a 70% lab-based, two-day experience designed to support providers in delivering high-quality, evidence-informed soft tissue care. Emphasis is placed on aligning information, expectations, and language with hands-on IASTM techniques to strengthen continuity of care, pain education, and the therapeutic alliance.
Participants will integrate current best evidence with decision-making frameworks, IASTM manual therapy techniques, and foundational pain science concepts. The course is built for immediate clinical application, supporting providers in confidently incorporating IASTM into comprehensive patient care.
By the end of the course, participants will be able to immediately apply evidence-informed clinical reasoning, IASTM manual therapy, and pain science education to improve patient outcomes.
Soft tissue work is not just about the tool — it’s about how, when, and why you use it.
The Dry Needling Network Technique and Protocol Library is your ultimate clinical companion – a comprehensive, ever-evolving repository of dry needling techniques, safety guidelines, and evidence-based protocols.
This is a subscription service created for clinicians who already have formal dry needling education, either through Revolution Human or another organization, who need a reliable, clinically sound source to review techniques before performing them in clinical practice.
Dry needling is precise work. Even for experienced clinicians, reviewing anatomy, hand placement, needle trajectory, patient positioning, and safety considerations before treating is part of responsible, evidence-informed care.
This library gives you on-demand access to technique videos designed to:
-
Refresh procedural confidence
-
Support safe and thoughtful application
-
Reduce variability and guesswork
-
Encourage preparation—not improvisation
These videos are intended as a review and reinforcement tool, not as standalone training or credentialing.
Use them to slow down, sharpen your reasoning, and walk into each treatment prepared.
This site will be updated regularly with new techniques and protocols!
This space was created to remove friction between clinicians and the evidence. Whether you’re new to dry needling or deeply experienced, having access to the literature matters—not to memorize papers, but to sharpen clinical reasoning and support better conversations with patients, peers, and regulators.
This is a free and open resource intended to:
-
Centralize key dry needling publications
-
Support evidence-informed practice (not dogma)
-
Encourage curiosity, critical thinking, and respectful discussion
You’ll find a range of studies here—from mechanistic work to clinical outcomes—reflecting the complexity of dry needling as a clinical tool. Use what’s here to question, refine, and strengthen how you practice.
If you come across high-quality research that belongs here, contribute it. This repository works best when it reflects the collective intelligence of the profession.
Glad you’re here—and glad you care about doing this work well.
Dry Needling Network (DNN) is a free collaborative community for clinicians to refine techniques, share cases, and push the profession forward. Learn, connect, share experiences, and lead alongside peers dedicated to elevating dry needling practice.
Get Excellence in Telehealth reframes virtual care as a powerful clinical environment—not a compromise. Participants will learn how to perform meaningful virtual assessments, deliver targeted and effective interventions, and build a strong therapeutic alliance through a screen using intentional language, presence, and clinical precision.
This course emphasizes real-time clinical reasoning—teaching providers how to adapt care dynamically, respond to patient cues, and maintain depth, trust, and outcomes in a digital setting. Participants will also gain practical tools for optimizing workflow, increasing patient engagement, navigating documentation and regulatory considerations, and delivering telehealth that is not only compliant, but truly human-centered and clinically impactful.
- Dry Needling
- Manual Therapy & Clinical Reasoning
- Digital Education
Category: Dry Needling
Integrated Clinical Dry Needling Total Body Level 1

Register here
The Integrated Clinical Dry Total Body Needling Course 1 provides clinicians with a comprehensive foundation in dry needling, including its historical context, proposed mechanisms, and current evidence supporting clinical use. Participants will develop proficiency in needle handling, CDC safety standards, pain education principles, and the clinical application of dry needling techniques for the most commonly treated and clinically relevant muscles.
The course also addresses state-specific rules and regulations governing dry needling practice. Clinicians will learn how to integrate foundational pain science concepts into real-world clinical decision-making. Instruction includes a detailed review of trigger points, patient positioning, and relevant anatomy — including vasculature, nervous tissue, and viscera — alongside safe and effective dry needling techniques and needle handling for all listed muscles.
This course is designed to support clinicians in delivering precise, informed, and responsible dry needling care grounded in anatomy, safety, and clinical reasoning.
The Integrated Clinical Dry Needling Course 2 is the second course in the two-part certification series and builds upon the foundational principles established in Course 1. This course provides clinicians with a deeper understanding of the history of dry needling, proposed mechanisms, and current evidence supporting its clinical utilization. Emphasis is placed on advanced needle handling and safety considerations, pain education, and the clinical application of dry needling techniques.
State-specific rules and regulations governing dry needling practice are reviewed to ensure safe, compliant application in clinical settings. Participants will further integrate foundational pain science concepts into real-world clinical decision-making.
Instruction includes an expanded review of trigger points, patient positioning, and relevant anatomy — including vasculature, nervous tissue, and viscera — along with dry needling techniques and needle handling for all previously introduced muscles as well as more advanced musculature.
Completion of Course 2 fulfills the requirements to complete the Dry Needling Certification.
Category: Manual Therapy
From Surgery to Sport: ACL Injury Rehabilitation With the Finish Line in Focus

A Revolution in Rehabilitation
Most ACL rehab courses teach you what to do.
This one teaches you how to think.
Join Dr. Luke Bunch, board-certified Orthopedic and Sports Physical Therapist and ACL rehab specialist, as he breaks open the black box of ACL recovery, from initial injury and early post-op decision-making to real-world return-to-sport demands.
With years of experience treating ligamentous knee injuries and mentoring rehab professionals, Dr. Bunch shares hard-earned insights that don’t live in protocols or timelines. You’ll gain practical skills, sharper clinical judgment, and a deeper understanding of how to guide athletes through one of the most challenging injuries in sports medicine.
Beyond clinical practice, Dr. Bunch is actively involved in ACL research and collaborates with leading clinicians and researchers across the country and internationally. His approach is grounded not only in day-to-day patient care, but also in ongoing scientific inquiry and dialogue with those shaping the future of ACL rehabilitation.
Learn how to think differently about ACL rehabilitation and change your outcomes.
Category: Manual Therapy
Unified Care: Integrated Clinical Reasoning and Patient Management for the PT/PTA Team

Physical Therapists and Physical Therapist Assistants work together across the full continuum of patient care. As research evolves and expectations rise, translating current best evidence into consistent, effective clinical practice can be challenging — especially within team-based environments.
The Unified Care: Integrated Clinical Reasoning and Patient Management for the PT/PTA Team course is designed to align physical therapists and physical therapist assistants around a shared framework for patient care. Emphasis is placed on continuity of care, effective pain education, strong therapeutic alliance, and the use of clear, appropriate language and communication to support optimal outcomes.
This 70% lab-based, two-day course integrates current evidence with clinical reasoning and hands-on manual therapy techniques for both peripheral and spinal joints. Participants will develop shared expectations, refine communication strategies, and practice manual skills that support cohesive, patient-centered care.
By the end of the course, participants will be able to immediately integrate evidence-informed clinical reasoning, manual therapy, and pain science education — working together as a unified team to deliver consistent, high-quality patient care.
Great outcomes don’t come from isolated providers — they come from unified care.
The Total Joint Post-Operative Care: Current Concepts and Best Practices course is a two-day experience designed to support evidence-informed assessment and treatment of post-surgical joint replacement patients. Through a combination of focused didactic instruction and hands-on technique labs, participants will expand their clinical skill set and exercise prescription strategies to influence muscle recruitment, tissue healing, and pain modulation — with the goal of improving functional mobility.
Participants will be guided through multiple examples of post-operative protocols, including stage-specific goals and progression strategies across the healing continuum. Emphasis is placed on understanding why and when to apply specific interventions, rather than simply following timelines.
By the end of the course, clinicians will be able to immediately integrate current best evidence, clinical reasoning, manual therapy, and pain science education into their existing rehabilitation approach for patients following joint replacement surgery.
Post-operative care isn’t about doing more — it’s about doing what matters, at the right time.
Category: Manual Therapy
Integrated Clinical Reasoning and Treatment of Dysfunctions: Lumbar Spine, Hip and Lower Extremity

Conditions involving the lumbar spine and lower extremity are a common source of pain, movement dysfunction, and long-term functional limitation. Effective care requires integrated clinical reasoning, skilled manual therapy, and movement strategies that address the system as a whole.
The Integrated Clinical Reasoning and Treatment of Dysfunctions: Lumbar Spine, Hip, and Lower Extremity course is a 70% lab-based, two-day experience designed to integrate current best evidence with decision-making frameworks and hands-on treatment. Participants will develop proficiency in manual therapy techniques — including joint mobilizations, high-velocity low-amplitude thrust techniques, neural mobilizations — alongside targeted exercise-based interventions for lumbar and lower extremity dysfunctions.
This course emphasizes immediate clinical application. Participants will learn how to assess, treat, and progress patients with lumbar spine, hip, knee, and ankle conditions using evidence-informed clinical reasoning. Foundational pain science concepts are integrated throughout to support thoughtful, patient-centered care.
By the end of the course, clinicians will be equipped to confidently apply current best evidence, manual therapy, and exercise strategies to improve function across the lumbar spine and lower extremity.
Lower quarter care isn’t about isolated joints — it’s about how the system moves, adapts, and recovers.
Conditions involving the cervical and lumbar spine are a leading source of pain, functional limitation, and long-term disability. Effective care requires more than isolated techniques — it demands integrated clinical reasoning, skilled hands-on treatment, and movement-based solutions.
The Integrated Clinical Reasoning and Treatment of Dysfunctions: Total Spine course is a 70% lab-based, two-day experience designed to bridge evidence, decision-making, and hands-on care for patients with cervical and lumbar spine dysfunction. Participants will integrate current best evidence with manual therapy interventions — including joint mobilizations, high-velocity low-amplitude thrust techniques, neural mobilizations — and targeted exercise-based strategies.
This course is built to support immediate clinical application. Participants will develop a clearer framework for assessment and treatment, refine manual skills, and learn how to integrate foundational pain science concepts into everyday clinical practice.
By the end of the course, clinicians will be equipped to confidently evaluate, treat, and progress patients with cervical and lumbar spine conditions using a thoughtful, evidence-informed, and human-centered approach.
Category: Manual Therapy
Integrated Clinical Reasoning and Treatment of Dysfunctions: Lumber Spine and Hip Region

Conditions involving the lumbar spine and the lower extremity frequently lead to impairments contributing to significant disabilities and functional limitations. This course is a 70% lab-based course integrating the latest evidence and frame work for decision making, and manual therapy for joints including high-velocity low-amplitude thrust techniques, neural mobilizations, and exercise based interventions for patients with lumbar and hip dysfunctions.
This 2-day course will enable the participant to understand and immediately integrate current best evidence, clinical reasoning, manual therapy, and exercises for the lumbar spine and hip. Additionally, they will be able to integrate the basics of pain sciences into their clinical practices.
Category: Manual Therapy
Integrated Clinical Reasoning and Treatment of Dysfunctions: Cervical and Thoracic Spine, Shoulder and Upper Extremity

Conditions involving the cervical and thoracic spine, shoulder, and upper extremity are a common source of pain, movement dysfunction, and functional limitation. Effective care requires integrated clinical reasoning, skilled manual therapy, and movement strategies that address the upper quarter as a connected system.
The Integrated Clinical Reasoning and Treatment of Dysfunctions: Cervical and Thoracic Spine, Shoulder, and Upper Extremity course is a two-day, lab-based experience designed to integrate current best evidence with decision-making frameworks and hands-on treatment. Participants will develop proficiency in manual therapy techniques — including joint mobilizations, high-velocity low-amplitude thrust techniques, neural mobilizations — alongside targeted exercise-based interventions for cervico-thoracic, shoulder, and upper extremity dysfunctions.
This course emphasizes immediate clinical application. Participants will learn how to assess, treat, and progress patients with cervical spine, shoulder, elbow, wrist, and hand conditions using evidence-informed clinical reasoning. Foundational pain science concepts are integrated throughout to support thoughtful, patient-centered care.
By the end of the course, clinicians will be equipped to confidently apply current best evidence, manual therapy, and exercise strategies to improve function across the cervical spine and upper extremity.
Upper quarter care isn’t about isolated regions — it’s about how the system communicates, stabilizes, and moves.
Instrument Assisted Soft Tissue Mobilization (IASTM) is a commonly used intervention across many clinical professions. As research evolves, effectively integrating current best evidence into day-to-day practice requires thoughtful clinical reasoning, clear communication, and consistent patient-centered care.
The Instrument Assisted Soft Tissue Mobilization course is a 70% lab-based, two-day experience designed to support providers in delivering high-quality, evidence-informed soft tissue care. Emphasis is placed on aligning information, expectations, and language with hands-on IASTM techniques to strengthen continuity of care, pain education, and the therapeutic alliance.
Participants will integrate current best evidence with decision-making frameworks, IASTM manual therapy techniques, and foundational pain science concepts. The course is built for immediate clinical application, supporting providers in confidently incorporating IASTM into comprehensive patient care.
By the end of the course, participants will be able to immediately apply evidence-informed clinical reasoning, IASTM manual therapy, and pain science education to improve patient outcomes.
Soft tissue work is not just about the tool — it’s about how, when, and why you use it.
The Dry Needling Network Technique and Protocol Library is your ultimate clinical companion – a comprehensive, ever-evolving repository of dry needling techniques, safety guidelines, and evidence-based protocols.
This is a subscription service created for clinicians who already have formal dry needling education, either through Revolution Human or another organization, who need a reliable, clinically sound source to review techniques before performing them in clinical practice.
Dry needling is precise work. Even for experienced clinicians, reviewing anatomy, hand placement, needle trajectory, patient positioning, and safety considerations before treating is part of responsible, evidence-informed care.
This library gives you on-demand access to technique videos designed to:
-
Refresh procedural confidence
-
Support safe and thoughtful application
-
Reduce variability and guesswork
-
Encourage preparation—not improvisation
These videos are intended as a review and reinforcement tool, not as standalone training or credentialing.
Use them to slow down, sharpen your reasoning, and walk into each treatment prepared.
This site will be updated regularly with new techniques and protocols!
This space was created to remove friction between clinicians and the evidence. Whether you’re new to dry needling or deeply experienced, having access to the literature matters—not to memorize papers, but to sharpen clinical reasoning and support better conversations with patients, peers, and regulators.
This is a free and open resource intended to:
-
Centralize key dry needling publications
-
Support evidence-informed practice (not dogma)
-
Encourage curiosity, critical thinking, and respectful discussion
You’ll find a range of studies here—from mechanistic work to clinical outcomes—reflecting the complexity of dry needling as a clinical tool. Use what’s here to question, refine, and strengthen how you practice.
If you come across high-quality research that belongs here, contribute it. This repository works best when it reflects the collective intelligence of the profession.
Glad you’re here—and glad you care about doing this work well.
Dry Needling Network (DNN) is a free collaborative community for clinicians to refine techniques, share cases, and push the profession forward. Learn, connect, share experiences, and lead alongside peers dedicated to elevating dry needling practice.
Get Excellence in Telehealth reframes virtual care as a powerful clinical environment—not a compromise. Participants will learn how to perform meaningful virtual assessments, deliver targeted and effective interventions, and build a strong therapeutic alliance through a screen using intentional language, presence, and clinical precision.
This course emphasizes real-time clinical reasoning—teaching providers how to adapt care dynamically, respond to patient cues, and maintain depth, trust, and outcomes in a digital setting. Participants will also gain practical tools for optimizing workflow, increasing patient engagement, navigating documentation and regulatory considerations, and delivering telehealth that is not only compliant, but truly human-centered and clinically impactful.